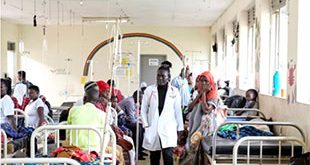
Dr Matovu says several interventions through research have been developed and now need to be put to use to reduce HIV/AIDS prevalence and new infections in Uganda especially for women, children and their families.
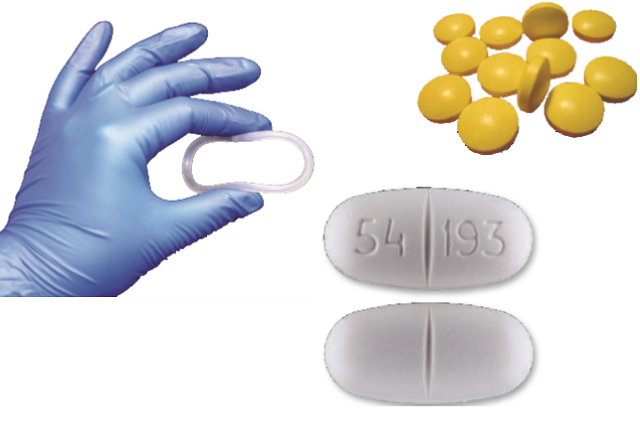
The vaginal ring
Matovu was involved in another intervention designed to empower women, the vaginal ring, which has been tested in Africa for fifteen sites. In Uganda 253 women were used in the study which revealed that for every 100 women who were given the active ring and used it (one that has dapivirine), 75% were protected.
The ring has not been officially rolled out, but the women who participated in the research were recalled and given an active ring for follow up over a period of one year to attain more data an adherence.
“We want to find out the protection levels if the person inserts the ring and whether it will go up but also find the adherence levels to ascertain whether women solely rely on the ring,” says Matovu.
The single-dose of Nevirapine
This was the first intervention on single pill that was given to HIV positive women at the onset of labour.
At the onset of labour, the pill was administered and when the baby is born, he or she was given syrup with 72 hours. This method save up to 50% and since then research has been building on to further reduce infection rates among children.
However Dr Matovu says the single dose remains obsolete as more research has been done including giving women ARVS and giving children syrup for as long as they are breastfeeding rather than just single dose when they are just born. This is all part of Prevention of Mother To Child Transmission of HIVB/AIDS (PMTCT).
The current standard according to Dr Matovu is to give ARV’s to the mother because if the viral load goes down, chances of infecting the baby are very slim minimal.
Oral PrEPs tablets for discordant couples
Matovu says they are soon rolling out oral preps for discordant couples. These are taken and given enough time like two weeks for the drug to accumulate enough in the blood so the person can be sure up to about 95% that they cannot get infected. One can then use a condom as a backup method until they are at no risk.
For children who are exposed, Matovu says the best intervention is for a mother to test; especially either before or as soon she ascertains pregnancy.
“When discovered positive, they are treated immediately and the intention is to make the viral load so low that the risk of infecting the baby is almost zero”.
She says therapy has moved from single pill interventions of women in labour to treating with ARVs.
“We realised that children who were saved in the 1990s are now getting infected which is why we have gone into not just protecting the mother but also the child,” she says.
Sugar coated tablets
Uganda has 950,000 children estimated to be HIV-positive, 62,900 of whom are on treatment. Of these, 3,000 are on second line and 48 on third line of treatment. An estimated 7,000 to 8,000 children who are born with HIV are on Nevirapine therapy. The sugar coated tablets have been made in form of pellets and the taste has been masked to ease use by children. The new formulation of Lopinavir/Ritonavir drug, which is prescribed as a second line treatment for children less than 15 years, replaces the bitter-tasting syrup formulation of the same drug. Matovu says such sugar coated pills are a good way to make children adhere to their treatment.
****
editor@independent.co.ug
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price