
Uganda’s scientists, researchers join race
Kampala, Uganda | PATRICIA AKANKWATSA | Uganda is among countries where researchers are working to develop a safe and effective vaccine against SARS-CoV-2, the novel coronavirus that causes COVID-19.
Prof. Pontiano Kaleebu, the director of Uganda Virus Research Institute (UVRI), says they are looking at two strategies to make sure Ugandans get the vaccine.
“We are looking at two ways; the first one is to see how our scientists can develop the vaccine locally. The other way is to partner with foreign researchers who are developing the vaccine and we do the clinical trial in the country,” he says.
He says partnering with foreign scientists who are in late stages of developing the Covid-19 vaccine can improve the country’s mileage on timely delivery of the vaccine. According to him, the institute could find a promising vaccine and start clinical trials by December.
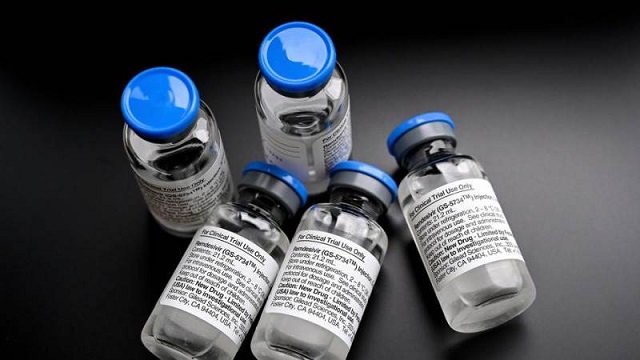
At the time he spoke, July 23, Uganda had just registered its first COVID-19 death, with 1078 confirmed cases, and 958 recoveries.
[UVRI has since confirmed that they are aligned with Imperial College of London to launch the country’s first COVID-19 vaccine clinical trial by December 2020.Professor Kaleebu and his team are authoring the protocol directing the trial associated with the vaccine under development by Imperial College London of the United Kingdom. The first phase trial will center on safety and immunogenicity.]
More than 15 million cases have been reported worldwide, while an excess of 8.6 million patients have recovered, according to figures compiled by US-based Johns Hopkins University.
Dr. Ekwaro Obuku; a physician and health policy expert, who recently headed the Uganda Medical Association, says Uganda’s hope for conquering COVID-19 lies in a vaccine.
“Vaccines are the next best discovery to man after learning how to trap and use oxygen to save lives,” Obuku says.
One of the vaccines being trialed so far is the mRNA-1273, which is being co-developed by researchers at the U.S’s biomedical and public health research agency, the National Institutes of Health (NIH) through its National Institute of Allergy and Infectious Diseases (NIAID) and the biotech company Moderna, Inc.
Scientists began Phase 1 trials of mRNA-1273 in mid-March. In April, researchers enrolled adults ages 55 years and older.
A larger phase 2 clinical trial of mRNA-1273, sponsored by Moderna, began enrollment in late May. During this phase, researchers will continue to evaluate vaccine dosing and immune response. Plans are underway to launch a Phase 3 trial later this month to test the vaccine’s effectiveness in thousands of people. Currently the Phase 1 trial has 120 participants.
Before a vaccine is available to the public, it must go through several stages of testing. The first stage is a Phase 1 clinical trial. In Phase 1, the vaccine is given to healthy volunteers to test if it’s safe and induces an immune response against the virus.
The two-dose vaccine is designed to prompt the immune system to produce antibodies against a portion of the coronavirus “spike” protein, which the virus uses to bind to and enter human cells.
The vaccine uses messenger RNA (mRNA), a molecule critical for the virus to produce protein.
The researchers, led by Dr. Lisa A. Jackson of Kaiser Permanente Washington Health Research Institute, Seattle, published an interim report of the trial findings in the New England Journal of Medicine on July 14.
“Finding a safe and effective vaccine to prevent infection with SARS-CoV-2 is an urgent public health priority,” said NIAID Director, Dr. Anthony S. Fauci, “The preliminary result of this trial is an important milestone toward this goal.”
The team tested the vaccine in 45 healthy adults, ages 18 to 55. Participants were enrolled at study sites in Seattle and Atlanta. The volunteers were divided into three groups. Each group received different doses of the vaccine (25, 100, or 250 micrograms). Participants received two injections, 28 days apart.
After the second injection, the team evaluated how well the vaccine provoked an immune response against SARS-CoV-2. They also tested whether the antibodies could neutralize the virus in the laboratory. Safety was assessed throughout the trial as well.
The investigational vaccine induced a strong immune response and was generally well tolerated. Antibody levels were higher with higher doses of the vaccine. In both the middle and high dose groups, the researchers observed high levels of neutralizing antibody activity through day 43 after the second injection. These levels were similar to the upper range found in patients who had recovered from COVID-19.
None of the participants experienced serious side effects from the vaccine. However, more than half reported fatigue, headache, chills, or pain at the injection site. These symptoms were most common following the second vaccination and in those who received the highest vaccine dose. Based on side effects and immune response, the 100 microgram dose was chosen for an upcoming Phase 3 trial.
****
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price





Thanks to the ugandan government. Sure this is promising.
Let’s wait for the vaccine to be released.