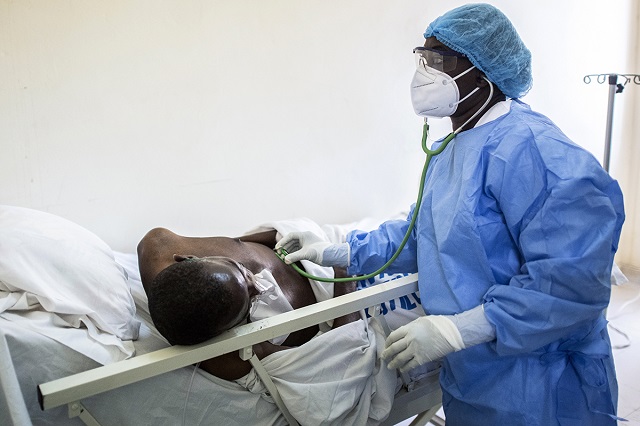
The Uganda case
No herd immunity models for COVID-19 in Uganda have emerged publically from the Ministry of Health, universities, or respectable scientific institution or individuals.
But Ugandan scientists attempted in the early days of the COVID-19 pandemic to design a model to predict the rate at which COVID–19 would spread. Their paper titled ‘A Mathematical Model Approach for Prevention and Intervention Measures of the COVID–19 Pandemic in Uganda’ was released in May 2020.
The scientists; Fulgensia Kamugisha Mbabazi, Yahaya Gavamukulya, Richard Awichi, Peter Olupot–Olupot, Samson Rwahwire, Saphina Biira, and Livingstone S. Luboobi, estimated the COVID-19 reproduction number in Uganda to be Rn0= 0.468.
The scientists constructed various mathematical scenarios. In one of these, they predicted the worst case scenario; the rate at which COVID–19 would spread in the country with zero prevention and intervention measures. Based on their calculations, 4,370 people would have been infected by June if there were zero prevention and intervention measures.
But while tracking and testing of suspected cases and contacts of confirmed infected people was minimal, unlike China, Europe and USA where the lock down followed high numbers of cases and deaths, Uganda imposed a lockdown as soon as the first cases were reported in March.
The government also introduced prevention and intervention measures that focused on social distancing, increased hygiene, and wearing masks. President Yoweri Museveni gave regular guidance and mass sensitization from the government in national television addresses. Reported cases of confirmed positive COVID-19 cases and deaths by the Ministry of Health remained low. By June 30 Uganda had recorded only 889 positive cases and zero death.
Although the Ugandan scientists did not make any herd immunity models, calculations based on their figures show that, at the time, about 53% of Ugandans or 24 million people needed to be infected for the country to get herd immunity.
By Sept. 18 the Case fertility Rate (which is the number of deaths by number of infections as a percentage), is 60 deaths recorded by 5380 confirmed positive cases as a percentage or 1%. Therefore, based on the rate of infection in May and the CFR of 1% as at Sept. 18, at least 240,000 people would have to die for Uganda to get herd immunity.
But the numbers could be even higher. That is because the rate of infection or Reproduction Number (RO) is no longer Rn0= 0.468. It is higher. That means a higher number of people need to be infected to reach herd immunity. And many more would have to die. Are we, as a country, ready for that?
The government says it is ready. And as part of its preparations, the Ministry of Health says it has converted parts of the Mandela National Stadium at Namboole into a 210-bed auxiliary hospital. The Ministry has taken journalists on tour of the facility and displayed row upon row of beds that look like graves in cemetery.
Based on this, and unlike in the past when the government introduced lockdowns and other COVID-19 prevention measures, the government is now busy opening up shopping centres and public transport. Now many observers fear COVID-19 infections could worsen as schools, places of worship, and borders open.
Most studies show that older persons are hardest hit by COVID-19. The Uganda 2020 population, estimated at 46 million people at mid-year according to UN data, is relatively young. It has a median age or 50% of the population aged 17 years and below. Only 2% of Ugandans are above 65 years old.
This has led to predictions of a relatively low COVID-19 impact on Uganda because of its young population, compared to China and the United States with a median age of 38 years and Europe 43 years.
But a look at other factors that could influence the spread and impact of COVID-19 in Uganda shows things could get gloomier very easily and rapidly.
According to the Washington DC-based Population Reference Bureau (PRB) which studies such issues, low capacity of health facilities, the opening up of cross-border and air travel, constrained sanitation, hygiene, social distancing in refugee camps, the high population densities in low cost urban settlements, and limited ability to monitor transmission rates and prevent spread could spell doom.
****
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price


