WHO, UNICEF places them behind Rwanda, Kenya, Tanzania
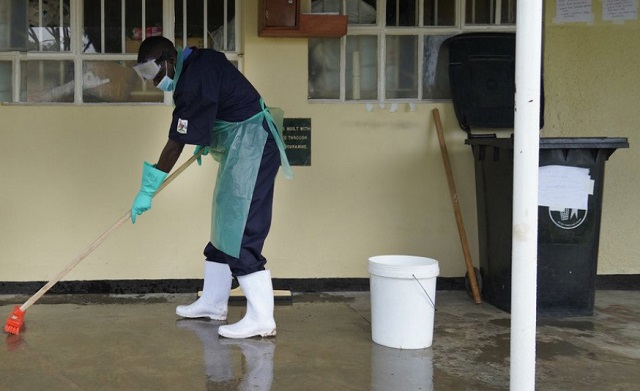
NEWS ANALYSIS | THE INDEPENDENT | Ugandan health facilities are listed among 8 countries with the lowest coverage of water, sanitation and hygiene (WASH) services in the world, according to the latest report by the Joint Monitoring Programme of the World Health Organisation (WHO) and the United Nations Children’s Fund (UNICEF).
Uganda is among 8 countries where basic coverage of water, sanitation and hygiene remained below 33% in 2021. Uganda has only 24% basic coverage. The other countries below the 33% mark are Niger, Malawi, Solomon Islands, Vanuatu, Honduras, Laos, and Sudan.
In the East Africa region, Rwanda has the best coverage at 65%, Kenya 42%, and Tanzania 45% basic hygiene service.
This 2022 update released in late August presents national, regional and global estimates for WASH in health care facilities up to the year 2021.
Among regions with sufficient data available to calculate regional estimates, coverage ranged from 53% in Northern Africa and Western Asia to just 38% in sub-Saharan Africa and in Eastern and South-Eastern Asia, while in LDCs only one in three health care facilities (32%) had basic hygiene services in 2021.
Service levels varied widely. Among 40 countries with available data, national coverage of basic hygiene services was at least 50% in just 22 but only 14 had reached 75% coverage. In Europe and Northern America, Serbia (86%) was the only country with data available that had not yet achieved universal access (>99%). In Northern Africa and Western Asia, coverage ranged from universal access in Azerbaijan, Kuwait and Oman to just 17% in Sudan while in Eastern and South-Eastern Asia coverage ranged from 93% in Thailand to just 16% in the Lao People’s Democratic Republic.
In sub-Saharan Africa, Rwanda, Ghana and Zimbabwe were the only countries with >50% coverage but none of the countries in Oceania met this threshold in 2021. In eight countries, more than one in four health care facilities had no hygiene service at all, including Sudan where two out of three health care facilities had no facilities at either points of care or toilets.
In 2021, 82% of health care facilities in Northern Africa and Western Asia had any hygiene facility and the remaining 18% were therefore classified as having no service.
Hand washing
In 2021, 62% of health care facilities had hygiene facilities with water and soap or alcohol-based hand rub at points of care. Health facilities with both hand hygiene at points of care and handwashing at toilets meet the criteria for a basic service. The health facilities with hygiene points either at points of care or at toilets, but not both, are classed as having a limited service.
In the majority of countries with data, access to hand hygiene facilities is higher at points of care than at toilets, but there are important exceptions. For example, in China two thirds of health care facilities (67%) had handwashing facilities with water and soap at toilets, but just one third (36%) had hand hygiene facilities at points of care. By contrast, in Uganda three quarters of health care facilities (74%) had hand hygiene facilities at points of care, but only a quarter (24%) had handwashing facilities at toilets.
There are also disparities in basic hygiene coverage between government and non-government health care facilities.
In Bangladesh, Sudan and the United Republic of Tanzania, basic hygiene coverage was over 30 percentage points higher in non-government health care facilities.
Promoting hand hygiene has been shown to positively influence compliance among health care workers and several countries collect information on the availability of promotional materials in health care facilities.
Ghana is one of the few countries with sufficient time series data to enable analysis of trends in hygiene services before and during the COVID-19 pandemic. Quarterly data from the District Health management Information System show that between March 2018 and December 2019 there was a steady increase in the proportion of health care facilities with a limited service while coverage of basic services showed little change.
Since the start of the COVID-19 pandemic there has been a marked acceleration, with coverage of basic services rising from 41% in December 2019 to 57% by June 2021. But over the same period, the proportion of health care facilities with no hygiene service remained largely unchanged at 2% .
The report points out that while the global indicator for basic hygiene services is universally relevant, it does not address other aspects of hygiene that are important for preventing and controlling infections and for providing high quality healthcare. It says it is therefore important to progressively incorporate other aspects of hygiene into national monitoring systems, especially where most health care facilities have already met the basic service level.
For example, Ireland requires health care facilities to monitor whether health care workers are complying with basic hand hygiene protocols and has established national targets for compliance. This enables analysis of trends in specific hand hygiene behaviours at the ‘five key moments’ defined by World Health Organisation (WHO) namely; before touching a patient, before clean or aseptic procedures, after touching a patient, after touching patient surroundings, and after body fluid exposure.
Reliable water supplies
Reliable water supplies are essential in health care facilities to allow washing of hands, environmental surfaces and medical equipment. Health care workers and patients also need access to water for their own personal needs, including drinking, washing and personal hygiene. It is impossible to deliver safe health care without abundant water, which is only possible when water supplies are available on the premises, and ideally piped through the facility.
By 2021, estimates for basic water services were available for 59 countries and three out of eight SDG regions, representing 37% of the global population. On this basis it is estimated that nearly four out of five health care facilities (78%) had a basic water service in 2021 (88% of hospitals and 77% of non-hospitals).
In Uganda, up to 99% of health facilities had either basic water supply or limited service. Only 1% had no water service. Basic service means water is available from an improved source on the premises, including piped water, boreholes, protected dug wells, protected springs, rainwater, and packaged or delivered water. Limited service means an improved water source is within 500 metres of the premises. No service means water is taken from unprotected dug wells or springs, or surface water sources; or an improved source that is more than 500 metres from the premises; or there is no water source. It is estimated that 79% of facilities in sub- Saharan Africa had an improved water source in 2021and the remaining 21% were classed as having no service. Uganda was at 52% basic and 47 limited service.
Routine environmental cleaning
Microbial contamination of surfaces in health care facilities can lead to transmission of Healthcare Associated Infections (HAIs), as well as contribute to the development of antimicrobial resistance (AMR). Robust systems for routine environmental cleaning are therefore essential to reduce the risk of HAI for patients, visitors and staff in health care facilities. This requires that staff with responsibility for cleaning floors and work surfaces should be identified, trained, provided with the necessary materials, and supervised as part of a broader approach to Infection Prevention and Control (IPC) within the health care facility.
None of the countries in sub-Saharan Africa and Oceania had reached 50% routine environmental cleaning coverage by 2021. This means none of the countries surveyed had sufficient and appropriate IPC supplies and equipment such as mops, detergent, disinfectant, personal protection equipment (PPE) and sterilization. They also did not have necessary power/energy required to enable performance of all basic IPC measures according to minimum requirements/standard operating procedures (SOPs), including all standard precautions as applicable.
In some countries, protocols are widely available but staff are not all trained. In Rwanda, for example, there was nearly a 50 percentage point gap between the proportion of facilities with protocols (92%) and with all staff trained (43%).
In Sudan, 1 in 5 health care facilities (21%) had no staff responsible for environmental cleaning, only 1 in 20 (5%) met the basic service level, and in 3 out of 5 facilities (62%) none of the staff had been trained. Non-government facilities were twice as likely to have protocols than government facilities (18% versus 9%), and five times as likely to have trained all staff (16% versus 3%).
Basic health care waste management
In 2021, estimates for basic health care waste management services were available for 65 countries.
A wide range of technologies are used to treat health care waste, and the most appropriate technology will depend on local circumstances, balancing the need to protect public health and the environment. It is recommended that waste treatment techniques that minimize the formation and release of chemicals or hazardous emissions should be prioritized. Incineration or burning is widely practised, but can cause serious environmental pollution, including the formation of highly toxic dioxin and furan compounds.
Basic waste management services calculates important aspects of waste management, such as the effectiveness of segregation practices or the reliability of treatment systems. Indicators might include whether used syringes are placed into safety boxes or de-fanged immediately after use, safety boxes are filled to appropriate level, Visual evidence and interview show that standard safety boxes are used, and the sharps container is PQS approved or complies with national policy.
In Uganda, visual evidence and interview showed that standard safety boxes are used, and the sharps containers are PQS approved or comply with national policy at about 60%. But used syringes are placed into safety boxes or de-fanged immediately after use in only about 10% of cases.
Sub-Saharan Africa was the region with the highest data coverage, with estimates from 24 countries representing three quarters of the regional population. A regional estimate could therefore be made, that 39% of health care facilities (55% of hospitals and 30% of non-hospitals) in sub-Saharan Africa had basic services in 2021. This means that 682 million people in sub-Saharan Africa lacked a basic waste management service at their health care facility, including 66 million people with no waste management service (neither segregation at points of generation nor safe treatment and disposal). In Guinea-Bissau and the Democratic Republic of the Congo less than 5% did, 3% in Sudan.
Calculation of the basic waste management indicator requires data on waste segregation as well as treatment and disposal of infectious wastes and sharps.
In many countries, a large proportion of health care facilities had some limited separation and/or treatment and disposal of sharps and infectious waste but did not meet all criteria for a basic service. Treatment levels were significantly higher than segregation levels in several low income countries, including the Democratic Republic of the Congo and Guinea-Bissau where almost no health care facilities segregated waste.
In most countries, basic waste management services are higher in urban than in rural areas. In Uganda about 40% had basic waste management services in rural areas compared to about 45% in urban health facilities. In Ethiopia the gap is over 60 percentage points. But in a few countries, this trend is reversed; in Mali, Senegal and Haiti, basic services were slightly higher in rural areas, usually because of higher waste segregation rates.
****
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price


Well, nice to look at the findings:
We get back to the report to the August House was any of this captured?
Hopefully the recommendation of the HCIV will factor in the needs that have been identified
BUT
If cleaning services are outsourced, why are the cleaners not trained?
Hygiene covers the person, environment and equipment; where is the problem? Any budget for this purpose?
How much is achieved in an over crowded health facility?
Is the supply of alcohol rub consistent, is it the right alcohol?
The soap , is the supply consistent?
So you have disposable needles and syringes in the box, how is transport and destruction?
An overcrowded and busy unit with a small work force and minimal supplies will definetely register shortcuts
The next time we read about antimicrobial resistance, awareness of its transmission by clients from the community into hospital, within hospital and from hospital back to community may be among the priorities: hygiene being a vital practice in breaking the chain of transmission
As we stand now the individual has to take responsibility for self and others around him
Hello.. I’d like to cite this but.. no author and citing details.. any help.. please