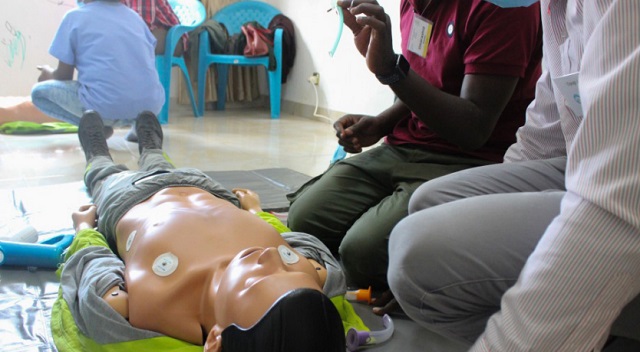
Uganda aims to create its first national emergency medical system. For now, the injured linger until help arrives — and hope it arrives in time.
Global Press Journal | PATRICIA LINDRIO Senior Reporter | Around 1:40 a.m. on April 6, Richard Kabunga was walking home from a friend’s housewarming party when he found a man lying unconscious outside a bar in his neighborhood.
“He had been left for dead by the roadside,” Kabunga says. “It was raining heavily, so his body was not only in shock but presented with symptoms of hypothermia.”
Kabunga works as a basic life support provider with the Red Cross. Immediately, he began performing CPR. “I pressed on his chest about nine times, and he came back,” Kabunga says. “I was so relieved and thankful to have been there at that time.”
David Wasswa, the man whose life Kabunga saved, still cannot remember exactly what happened that night. He and his friends had been drinking at the bar when an argument broke out with a group of other men. The situation escalated, and the men began punching and kicking Wasswa, who fell to the ground. As he lay motionless, the crowd scattered into the night. His friends believed he was dead — and he might have been, if Kabunga had not found him.
“My head still hurts, and my body is sore, but at least I am breathing,” Wasswa says.
Many Ugandans are not so fortunate. Outside of hospitals, the country’s emergency care system is almost nonexistent. Without a dedicated fleet of ambulances or trained emergency medical technicians, Ugandans who get into serious accidents or find themselves in life-threatening situations often are left to fend for themselves and hope for the best.
The Ugandan government aims to change this through a National Medical Services Policy, which would create the country’s first official emergency medical service system. The policy would establish a national emergency call and dispatch center, allocate funding for a fleet of ambulances, and provide training and equipment to emergency medical technicians (EMTs).
The Ministry of Health, together with the Ministry of Works and Transport, also is working to update the country’s traffic laws so that ambulances are required to carry stretchers, oxygen, defibrillators and other lifesaving equipment, and ambulance drivers are required to hold special licenses.
“We didn’t have standards for ambulances,” says Maria Nkalubo, principal operations officer at the Ministry of Health. “It was basically scoop and run.”
Patients are typically driven to hospitals in whatever vehicle is available, including cars, taxis and motorcycles. Drivers lack medical experience and, without trained EMTs, there typically is no clinical documentation of patients’ symptoms, Nkalubo says.
Joshua David Kavulu, a medical officer at Lubaga Hospital, says that having EMTs who can treat patients in the field and on the road will greatly improve the outcomes for patients after they arrive at medical facilities.
“Pre-hospital care is important, because it determines hospital prognosis,” he says.
Such training should become standard, agrees Peter Kavuma, managing director of Emergency Care Courses Uganda, an organisation that provides training in CPR and other lifesaving techniques to health care workers and members of the public. He is helping to draft the new national policy.
“All ambulance personnel should be skilled in life-and-death training, but you find that even health professionals are not trained in that,” he says. “Emergency units are nonfunctional. They do not know what to do! That is scary.”
To address the situation, the government has approved a new two-year course to train EMTs, but Nkalubo says the government should allocate more money in the budget for equipment, medicine, a call center and emergency vehicles.
Nkalubo estimates that the country will need at least 425 ambulances, approximately 1 for every 100,000 people in the country. So far, the government has obtained only 119 ambulances.
“We need to procure more ambulances,” she says, but didn’t specify how much money would be required to fund the new EMS operations.
The African Federation for Emergency Medicine estimates the total cost of emergency services in Uganda during the 2018-19 financial year was Shs60 billion (about $16.9 million). In contrast, the Ministry of Health allocated just Shs958 million (about $270,000) for emergency services that year out of a total health care budget of Shs2.3 trillion (about $648.1 million).
Still, the government’s plans come as a relief to Marion Atuhaire, who got into a serious car crash in 2018 while she was on her way to work. With no emergency number to call or dedicated ambulance to assist her, all she could do was wait for help to arrive.
“I remember waiting in the roadside ditch for what seemed like an eternity, people talking over me, cars moving — life was going on as usual,” she says.
Eventually, she was pulled from the wreckage and taken to the hospital in a police truck. Atuhaire injured her spine in the crash and must now use a wheelchair.
“I will never forget the pain from when they carried me onto the police truck,” she says. “I felt broken. It was so traumatic, and I don’t wish that on anyone.”
****
Patricia Lindrio is a Global Press Journal reporter based in Kampala, Uganda. She specializes in health and migration reporting.
Source: Global Press Journal
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price


