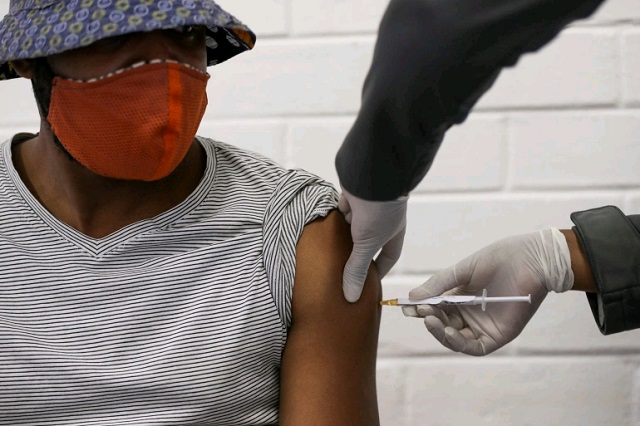
Realistic assumptions for policymakers to build into their vaccination planning
| SWEE KHENG KHOR | Vaccinating the world against COVID-19 is one of mankind’s most critical non-wartime efforts ever. Many countries have developed ambitious, politically sensitive, and carefully sequenced vaccination plans, but executing them successfully will be a challenge. To succeed, policymakers should build three realistic assumptions into their vaccination planning for 2021 and beyond.
First, delays are inevitable. More than two months after the world’s first COVID-19 vaccine injection on December 8, 2020, hopes of a rapid rollout are fading in many countries. Production holdups have triggered European Union threats of legal action and export restrictions. And there are several reasons to expect further delays.
For starters, the manufacturing constraints are daunting. Firms must scale up or repurpose factories to produce billions of doses annually, and vaccine supply chains are still being built even as they are being stretched. For example, the Pfizer/BioNTech and CureVac vaccines use lipid nanoparticles manufactured by the same supplier.
Moreover, capacity expansion through technology transfer – say, from AstraZeneca to Thailand’s Siam Biosciences – involves legal and technical hurdles. If new coronavirus variants reduce current vaccines’ effectiveness, vertically integrating the research-to-manufacturing process may enable a faster and more agile response.
Other legal and regulatory obstacles also could cause delays. Many countries have signed bilateral advance purchase agreements (APAs) with vaccine manufacturers, most of which are subject to the vaccine gaining regulatory approval and involve phased delivery and a refundable deposit. But APAs may be difficult to enforce, and international law must evolve rapidly for dispute resolution to be effective.
The United Kingdom’s regulator was the first to approve the Pfizer/BioNTech vaccine because it benefited from rolling data submissions from clinical trials – an opportunity that should be accorded to other regulators, regardless of market size or wealth. A new approval process may be needed for vaccine variations in response to new coronavirus variants, perhaps modeled after the abbreviated approval pathway for seasonal variations in influenza vaccines.
Furthermore, a population-wide COVID-19 vaccination program poses formidable logistical challenges and will require an all-of-society effort. Governments may need to provide around-the-clock or drive-through vaccination facilities, with proper cold-chain support, while a robust adverse-event reporting system must accompany adequate indemnity protections. Wastage, sabotage, and weaponised vaccine hesitancy may occur. But countries can mitigate these potential problems by planning properly and learning from one another.
The second assumption is that COVID-19 vaccines will aggravate global inequality in 2021. All OECD countries except Turkey have procured more doses than their population needs; Canada, for example, has enough for nearly six times its population. This “vaccine apartheid,” as UNAIDS Executive Director Winnie Byanyima calls it, means that rich countries will most likely achieve widespread vaccination coverage and economic recovery sooner, leaving poor countries far behind.
COVID-19 vaccination programs could also worsen inequalities within countries, just as the pandemic itself has already disproportionately affected ethnic minorities, women, immigrants, and the poor. The World Health Organisation recommends vaccinating frontline health workers and the elderly first, but some advocate giving priority to ethnic minorities or the poor. Indigenous communities, migrants, and refugees could be marginalised further.
Meanwhile, wealthy elites could secure early vaccinations through the private sector, the black market, or “vaccine tourism.” Big businesses may purchase vaccines for their employees or lobby for them to be given priority as “essential workers”; Amazon and Uber are already doing so. And “vaccination passports,” if implemented, could be discriminatory.
Mitigating this inequality risk will require a multi-layered approach. The United Nations General Assembly and Security Council must govern global public goods more actively, while U.S. President Joe Biden’s administration needs to provide thoughtful and inclusive global leadership. Governments must sustain the financial and political support that the COVID-19 Vaccine Global Access (COVAX) Facility needs to make vaccines available everywhere in the world. The UN Human Rights Council’s Universal Periodic Review process for all member states could be expanded to include country-level COVID-19 outcomes and vaccine equity. And citizens, civil-society groups, and media must remain vigilant to prevent unequal vaccine distribution.
Lastly, policymakers should assume that procurement decisions could become a proxy for the US-China rivalry. Geopolitics is already influencing public procurement, notably in some Western countries’ decision to bar the Chinese telecommunications firm Huawei from their 5G networks. When it comes to vaccines, geopolitics could encroach on decision-making criteria like data, quality, availability, value, and cost.
Vaccines could also feature in the US-China competition over global standards, which already encompasses artificial intelligence, smart cities, and lithium batteries. COVID-19 vaccines may require new standards for research methods, primary endpoints in trials, clinical outcomes, and production. Just as the U.S. and the Soviet Union engaged in space and arms races during the Cold War, America and China could enter a vaccines race with the aim of gaining scientific prestige, standard-setting authority, soft power, and financial rewards.
Competition is good if it gives countries a choice of cheap, cutting-edge vaccines. But it could turn ugly if superpowers weaponise vaccine supplies, prices, or patents, or use them as bargaining chips in “vaccine diplomacy.”
If that happens – if choosing vaccines means choosing sides – small and medium-size powers can adopt a hedging strategy or “vaccine portfolio” approach, as Australia, Malaysia, and Singapore are doing already. But this could still leave countries caught in a bind if they are forced to choose whether to weight their portfolios toward the U.S. or China. To escape the bind, such countries could use international mechanisms like COVAX, or band together for pooled procurement using models like the Pan American Health Organisation’s Revolving Fund or UNICEF’s initiatives to strengthen vaccine procurement.
COVID-19 vaccines offer a welcome glimmer of hope after a bleak first year of the pandemic. But translating this hope into effective action will require policymakers to be resourceful in mitigating delays, inequality, and geopolitical risk.
****
Swee Kheng Khor, a Malaysian physician specialising in health policies and global health, holds fellowships at Chatham House, the United Nations University, and the Institute of Strategic & International Studies (ISIS) Malaysia.
Copyright: Project Syndicate, 2021.
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price




