 V
V
Study will involve 250 female participants from different parts of the country
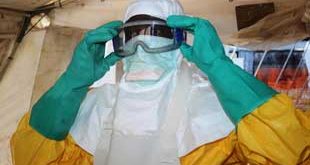
Kampala, Uganda |FLAVIA NASSAKA| Makerere University scientists working on finding effective treatment for HIV/AIDS are marking another milestone with the start of trial of injectable Antiretroviral (ARV) therapy.
In a joint project with scientists from the Johns-Hopkins University of USA, they are recruiting participants for the study expected to kick off in October.
The initiative aims at ensuring people have a range of choices for treatment by establishing a possibility of injectable ARTs for people whose tolerance of tablets is low.
At a science café organized by the Health Journalists network in Kampala, Dr. Flavia Matovu Kiweewa, a Senior Researcher told The Independent that the new study is not about whether the injection works or not because tolerance and its safety have already been confirmed. What they want to establish is how effective it is compared to other drugs that are already being used.
The study will involve 250 female sex workers sourced from different parts of the country. It will not include vulnerable groups like pregnant and breast feeding mothers.
Kiweewa says participants will be initiated on either ARV tablets – Lamivudine and Truvada or an injection – with a combination of drugs Carbotegravir and Rilpivirine.
“The studies have been submitted to regulatory authorities. With the popularity of injections in Africa, we thought injectables are more effective both as PrEP (pre-exposure Prophylaxis – a drug given to prevent HIV among people who are at risk of infection) and treatment especially among women who are less empowered,” she said adding that they picked lessons from the injectable contraceptive which has become the most widely used method.
A similar study has already been done and results were presented at the International AIDS Society conference held in Paris from July 23 to 27. The results showed that people involved had their CD4 going up and those who were not feeling well became OK clinically. The trial was conducted at 50 centers in the U.S., Canada, Germany, France and Spain and showed patients who used injections every after four weeks suppressed the virus at 87% whereas those who took an injection every after eight weeks had their virus suppressed at 94%.
The design is that a participant will initially be given oral drugs and then given an injection of 600mls every after eight weeks. The intention is for the researchers to be sure that one is infected in order to avoid resistance. For those who will use it as PreP, the injection will be given at the time when one expects to be at risk.
Treatment as prevention
Kiweewa is optimistic that once found effective, the injection will avert thousands of infections and save many lives. “When people know the product works, they are able to use it”, she says citing the vaginal ring whose acceptability has been rising since the first study with the latest showing effectiveness of over 70%.
Kiweewa says a person living with HIV will be given an injection that will last two months something that will solve complications that come with poor adherence such as resistance that are caused by skipping tablets that are supposed to be swallowed daily.
“With everyone getting on treatment, we need easier ways. The next step is to have more user friendly ways to ensure patients take their drugs.”
Drugs have proved to be effective both as treatment and prevention. In fact drugs have almost halved deaths related HIV and increasingly it’s becoming rare to find a child born with the virus. If injection is approved, even more people will be saved. And, the news has caused excitement. For Moses Nsubuga who has lived with the virus for over 20 years such advances in research show we are closer to finding a cure. He being on second line ARVs takes a cocktail of seven drugs daily – aluvia, septrin and combivir. His choice would be trioday – one tablet day if only he was on first line. “My doctors have never changed my medication. They say never change a winning team but all these drugs taken daily are huge for a human being”, he laments adding “Whenever we hear of fixed dose interventions we get excited but they are nowhere to be seen here. We need a combination that will ease our treatment journeys.”
For Charles Brown of the Infectious Diseases Institute (IDI) if an injection is added to the HIV treatment plan, it means clients will have a choice to pick what’s best for them. To him choice is very important especially if someone is to adhere to the regimens.
“People will still have choice to take an injection or pills and with more advancement in research longer lasting initiatives such as implants will be invented. At the IAS conference for instance one scientist told us they are studying a drug that is able to expose the hiding strains of HIV. This drug they said will be used after one takes ARVs to undetectable levels”.
Brown however warns that people shouldn’t be excited as yet as the various stages of clinical research take time to translate into something that can be rolled out for general use.
***
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price



Does HIV and AIDS really exist?
Specialized article by Prof. L. Dayeng, founder of the scientific research center of the Dayeng Foundation.
So-called AIDS drugs block the DNA copying process on the cell level, and thus a vital process. Any healthy or sick person, whether “HIV-positive” or not, will die in a very short period of time under aggravating conditions. Mostly within one to two years. Very few people have survived this “cure” for more than 3 years.
What is happening here? If there is really evidence that a HI virus exists that produces AIDS, scientific documents should still exist. But, there are no such documents.
Originally Posted by Dr. Heinz Ludwig Sänger, Professor of Molecular Biology and Virology from the Max Planck Institute for Biochemistry, (Germany): “To date, there is not a single scientifically convincing proof of the existence of HIV.” We advise anyone who has been tested positive for HIV to do the following. Request a clear proof of a so-called HI virus. You will soon discover that Niemad can show you such a virus.
All HI virus models you know from the media are not real photos, but computer graphics. In fact, a HI virus has not yet been detected. The acceptance of this simple fact is difficult for many people. After all, there are so-called HIV tests. Even with this theme, everything is different than most people think. In these so-called HIV tests, a certain virus is not detected, for example, a virus is not searched for. It is only searched for increased activity of antibodies. What does that mean? If a person suffers harmless viral infection at the time of the HIV test, he is likely to get a positive test result for HIV. Examples of relatively harmless antibody activities include: naturally occurring antibodies, influenza, vaccination, upper respiratory infections, current viral infections, antibodies to rheumatoid arthritis, lymph node swelling, blood transfusion, herpes disease, tetanus vaccination, renal failure, hepatitis, and hepatitis B, cancer diseases and so on. It is therefore sufficient for an increased antibody activity to make you an AIDS patient. There is currently no recognized standard for the detection of HIV infection, even the manufacturer of these tests makes this statement itself. Of course, no corresponding test can exist, as no HI virus (HIV) has been found so far. The manufacturer Hexal will now provide even healthy people with immune-debilitating drugs. So very slowly: Healthy people should prophylactically consume drugs for a disease that does not exist. This is a fantastic move from the pharmaceutical industry to make even more billions of profits. The people who still do not understand what is going on in classical medicine will inevitably become victims of an outstandingly organized business.
We, the independent, scientific research center of the Dayeng Foundation, have examined many so-called “AIDS sufferers” in 6 countries. We have never found a so-called HI virus (HIV). We have found several known viruses in some of the investigated ones, but they do not have any relevant, negative properties. We found no viruses in most of the investigated AIDS patients. However, we found a very weak immune system in all the investigated people. Only the so-called AIDS drugs were responsible for this immune deficiency. From our scientific knowledge, we have developed a therapy to stabilize and repair the immune system destroyed by the drugs. The results were and are that all treated patients (alleged AIDS sufferers), after therapy, were healthy.
You can now decide if you still believe in an industry that makes billions of profits on so-called AIDS drugs, or trust independent scientists whose only goal is to really help people. Decide quickly before your life ends. Another general good advice: Avoid pharmaceuticals if you want to stay healthy. Pharmaceuticals have never cured a disease, on the contrary, pharmaceuticals are responsible for most diseases. Now many people still say: “That can not be anything.” Think about the following. Why should so many international scientists, including Nobel laureates, claim something that is not true? What advantage would have all these scientists to publish it wrong facts? Further, think about why this industry, which makes billions of profits on AIDS drugs, can not show a HI-Virus. If it is about your own life, then you should ask yourself some of these questions. By the way, did you know that most of the financial resources of the World Health Organization (WHO) come from the pharmaceutical industry?
Prof. Dr. L. Dayeng, independent, scientific research center
how can i get that treatment
very simple, ask here: http://www.lupus-trust.net
Dr Harrison Can cure HIV/AIDs,
He cured me of HIV that has been in my system for almost Five years!
I also believe there is nothing relating to problem or sickness,he would be able to do same with his Spell Powers and solve your Problems!
Contact him on his Mail:-J.HARRISONSPELLHOMES@GMAIL.COM
Whatsapp No +1 (604) 337-1439
Avoid Scammers,I was also Scammed Severally!!!…
Nice advertisement, but maybe you can tell me what AIDS actually is and of which virus it originates. Please show me such a virus, but no computer animation.
You want to know what AIDS really is and who makes a profit from it? You can see it scientifically here: http://lupus-trust.net/interesting-facts/