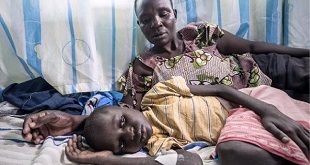
Kampala, Uganda | THE INDEPENDENT | A leading public health researcher and expert has criticized government for absconding from a responsibility to provide quality health care to citizens.
Associate Professor Sarah Ssali, a senior lecturer of Gender Studies at Makerere University and a Global Public Health specialist, says her research shows that Ugandan citizens have been turned into clients whose access to healthcare is determined by their own ability to pay, their location and socio-economic status.
Ssali notes that despite the reforms made in the health sector for the last 30 years, they are eroded the by little state responsibility in providing healthcare to citizens who are now exposed to vagaries of the market. She contends that the health sector in Uganda continues to be elitist, urban based and serves those with the ability to pay.
Presenting a paper titled “Neoliberal health reforms and citizenship in Uganda”, Ssali stated that health sector restructuring has contributed to the exclusion and marginalisation of wider sections of the population from accessing medical care. She advises that if equity concerns are to be achieved, the state and not the market, needs to be responsible for the citizen’s health.
She notes that the current free market economy has created winners and losers as well as re-fashioning citizens into clients in their own country.
“The winners, who with their newly acquired wealth can afford state-of-the-art diagnostic healthcare in and outside the country from facilities whose consultations are not less than UGX 60,000; and the losers, the under-privileged, who cannot even access the most basic of health services without depleting their few household resources,” Prof. Ssali observes.
Adding that; “The demographic majority of Ugandans are losers in this health system. They are stuck with poor quality services or can only access healthcare from private facilities by engaging in catastrophic expenditures.”
According to Ssali, out-of-pocket health expenditure continues to rise from 91% in 1997 to 97.3% in 2015.
“This high household expenditure and limited insurance cover could explain the increasing catastrophic health expenditures and subsequent household poverty and impoverishment that have been noted by the Ministry of Health,” she argues.
A 2014/15 Annual Health Sector Performance Report indicated that while the Ministry of Health had registered improvement in all impact factors, they were yet to register improvement in the percentage of households experiencing catastrophic expenditures on health services.
A breakdown of households’ out-of-pocket payments shows that most of it went to medicines, followed by hospital clinic charges, consultations and traditional doctors’ fees/medicines.
Ssali notes that as a result of the rising cost of health care especially consultation fees and high hospital or clinic charges, majority of citizens are resorting to self-medication or cheaper public healthcare, devoid of quality.
A regional dis aggregation shows that household healthcare costs increased for all regions. However, the increment was highest in the central Uganda, followed by western, eastern and northern region.
The study reveals that the rich and those residing in the central region, with more privileged access to income and healthcare, were more able to pay for the ever-rising costs of healthcare compared to those residing in the more rural and post-conflict northern regions.
Ssali discloses that donor funds have been directed towards sectoral programmes – typically for communicable diseases like HIV and Malaria – rather than preventive healthcare.
Government expenditure on health continues to be less than 10 per cent (or US$27 per capita) below the 15 per cent (or US$44 per capita) recommended by the Abuja Declaration.
Donors remain the main source of financing for the health sector. While about 97 per cent of healthcare costs are borne by households, which makes these expenses one of the most burdensome for the poor.
The limited funding for Primary Health Care –PHC activities could according to Ssali partly explain why several years after the reforms, preventable illnesses such as malaria, malnutrition, respiratory tract infections, AIDS, tuberculosis, perinatal and neonatal conditions remain the leading causes of the disease burden, as was the case in 1988.
She contends that the neglect of preventive healthcare has had a negative effect on the poor and it partly explains the sustained high incidences of preventable diseases and associated high mortality rates.
******
URN
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price