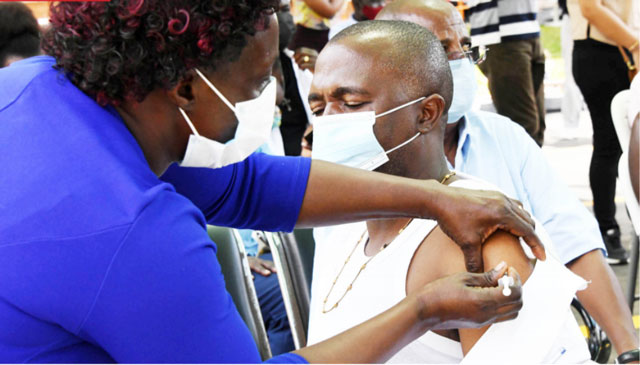
CORONAVIRUS 2ND WAVE: How will Uganda cope without vaccines?
THE INDEPENDENT | RONALD MUSOKE | The let-up in COVID-19 infections at the beginning of this year could have made many Ugandans think that they had finally won the battle against the disease. This was mainly because of the low number of positive cases that the Ministry of Health was reporting despite the busy political campaign season and end of year festive season euphoria.
But senior health officials now say the last four weeks have seen a drastic change in the rate of infections. They say Uganda is now officially under a second wave of the pandemic.
While, during the first wave, it took the country 3-4 months to get to the full-blown pandemic, in the second wave; it has taken Uganda just days.
Hundreds turn up for vaccination at the @MinofHealthUG this morning. This is the way to go! #ActOrPerishUG pic.twitter.com/b6Jfe5bSp0
— Maurice Mugisha (@MauriceMugisha) May 28, 2021
Dr. Yonas Tegegn Woldemariam, the World Health Organisation Country Representative says Uganda registered 256 positive cases of COVID-19 in the week starting April 25; a week later, on May 2, that figure rose to 411 and, by May 9 that figure shot to 475 cases. A week later, on May 16, cases registered nationwide were a whopping 1,060. The Ministry says there has been a particularly sharp rise in cases of COVID-19 in schools.This is the most worrying.
As of May 18, a total of 29 schools from 17 districts had recorded 803 cases and one death, according to Dr. Henry Mwebesa, the Director General Health Services. He told the media at the Ministry of Health headquarters in Kampala on May 27 that the affected schools include ten nursing schools, eleven secondary schools, seven primary schools, one Primary Teachers College and other tertiary institution (Kyambogo University).
But Mwebesa said some schools were not reporting cases because of fear they will be closed. “That is not our objective; our objective is to go there, investigate and if we can isolate those who are sick, treat them and those who are not, are allowed to continue,” he said.
The districts that have reported the highest number of cases in the last 14 days are; Kampala, Wakiso, Gulu, Amuru, Moroto, Arua, Mbale, Masaka, Oyam and Kalungu. However, Mwebesa said, this does not mean that the other districts are not affected. Rather, he said, it could imply the above mentioned districts have been vigilant in carrying out surveillance testing and reporting.
“This calls for vigilance and maximum responsibility from all of us to avoid being another statistic in this deadly pandemic,” Mwebesa said.
COVID-19: Museveni back on TV, Radio tomorrow 8pm https://t.co/vG0IJBuUff
— The Independent (@UGIndependent) May 28, 2021
Mwebesa said the main drivers of transmission in schools and other public spaces are overcrowding and non-adherence to public health prevention measures.
Mwebesa said, with the exception of supermarkets, banks and public offices, many other public spaces have been flouting the Standard Operating Procedures (SOPs) instituted in March last year when the country went into lockdown.
He said: “If you go to (the open) markets, the way people are behaving, people are overcrowding without wearing masks and there are no hand-washing facilities. You all know about the parties going on; some with over 1000 guests and the funerals are attracting as many as 2000 mourners.” He said even public transporters; especially bodabodas, are not wearing masks and carry up to three passengers.
Young people hit
Health ministry officials are worried that unlike the first wave which saw more elderly people under attack, young people are being infected at faster rates this time.
“Our data shows that the most affected are in the age groups of 20-39 years old and the intensity of severe and critically ill COVID-19 patients is higher than what we experienced in the first wave of the pandemic,” Mwebesa said.

Diana Atwine, the Permanent Secretary in the Ministry of Health says each time the virus mutates, it gets more aggressive and virulent.
“This can explain why we are seeing more people in ICUs suffering from severe illness yet they fall in the age groups that we initially thought were safe.
“So this business of saying that for me I am younger, I don’t have hypertension or diabetes and therefore I am safer and don’t need to get vaccinated should get out of our heads.
“We need to make sure that we all take precaution and make sure that we avoid infection because you don’t know how your body will react even when you are young or even when you don’t have any co-morbities.”
Dr. Misaki Wayengera, the chairperson of the Ministerial Scientific Advisory Committee on COVID-19 says experts are also seeing a faster progression of disease from the time someone gets exposed to the time they begin to develop symptoms.
He says, during the first phase of the pandemic, one could get some cough, then develop flu-like illness and then subsequently lose the sense of taste and smell.
“But given the fast progression, there is now a likelihood of missing some of these symptoms,” he said.
He said while the country was previously dealing with more or less an imported epidemic, “right now the virus is amongst us, it is moving and circulating amongst us.”
“We are seeing variants associated with more transmission and because of that we are noticing a fast rise in the curve for infections. We are seeing the variants affecting and killing younger ones.”

“This goes in far as saying that the second wave is here,” said Dr. Woldemariam, the WHO Country Representative, “The public health measures alongside getting vaccinated remain important interventions.”
Vaccination picks up as vaccines reduce
Meanwhile, following three months of hesitancy, officials at the health ministry say more Ugandans have over the last few weeks been coming out in large numbers to get vaccinated and the stock of vaccines is fast reducing.
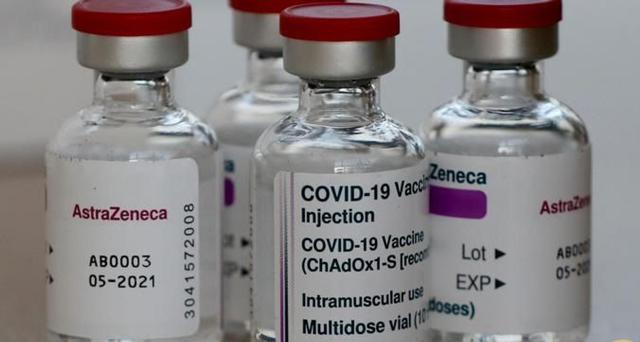
Dr. Mwebesa said by May 27, about 550,626 people had received the AstraZeneca vaccine meaning that about 400,000 doses are left to service millions of Ugandans who will need them over the next couple of weeks.
When the government first launched its vaccination programme against COVID-19 in March this year, Dr. Jane Ruth Aceng, the former Minister of Health said, she had earmarked 22 million people or 49.6% of the population for vaccination. She said each phase would see about 4.3 million people in the country aged 18 years and above eventually get vaccinated.
Dr. Aceng noted that the government had categorized people according to priority and risk of infection. The first group comprised 150,000 health workers, 250,000 security personnel and about 550,000 teachers. Others included about 550,000 people with underlying health conditions such as hypertension, Asthma and Diabetes.
To ensure that all these people are vaccinated, she said about 3,552,000 million doses would arrive in the country by June, this year, including the 964,000 doses that arrived in March from the Selum Institute, the India-based AstraZeneca vaccine manufacturer.
But, in April, India got hit with a second wave of virulent strain that saw the Indian government halt exports of the AstraZeneca vaccine so that it satisfies the home population first.
Dr. Woldemariam, the WHO Country Representative told the media that the consignment which Uganda was expecting in May has not come. The earliest it could arrive is in late June.
“We are working towards seeing how we can get alternative supplies other than India,” he said. He said there are now “efforts” globally for big countries that have excess vaccines to donate to more needy countries like Uganda.
He says the U.S., the U.K, Germany and Norway have recently come out to say they will be donating some of their excess vaccines to the COVAX Facility.
“We are working to see how we can benefit from those donations. But also some countries that have not been able to use their vaccines are returning them for redistribution.” He, however, noted that it is not automatic that Uganda will be eligible to get the donations.
The WHO Representative says it is important that Uganda’s rate of vaccination improves. He said the reason as to why Ghana and Kenya have, for instance, been able to get their second consignment quickly from the redistributed vaccines is because of their relatively better successful vaccination programmes.
“Uganda could have benefitted as well had its vaccination effort been good. It is important to go out and get vaccinated.”
Richard Kabanda, the Acting Commissioner in charge of health promotion, communication and education blamed the poor vaccine intake on alarmist social media messages coupled with limited public awareness. He said the risk perception based on the number of positive cases has an effect on how people perceive the need to get vaccinated.
Africa struggles to stock vaccines
According to the World Health Organisation regional office, Africa needs at least 20 million doses of the Oxford-AstraZeneca vaccine in the next six weeks to get second doses to all who received a first dose within the 8— 12-week intervals.

“As supplies dry up, dose-sharing is an urgent, critical and short-term solution to ensuring that Africans at the greatest risk of COVID-19 get the much-needed protection,” said Dr Matshidiso Moeti, the WHO Regional Director for Africa. “Africa needs vaccines now. Any pause in our vaccination campaigns will lead to lost lives and lost hope.”
“It’s too soon to tell if Africa is on the cusp of a third wave. However, we know that cases are rising, and the clock is ticking so we urgently appeal to countries that have vaccinated their high-risk groups to speed up the dose-sharing to fully protect the most vulnerable people.”
In the meantime, Dr. Mwebesa said, the Ministry’s COVID-19 Strategic Committee in consultation with the Scientific Advisory Committee had resolved to withdraw COVID-19 vaccines from the districts that have not fully utilized them so they get redeployed in districts that need them more.
He said whereas districts in southwestern Uganda have performed very well and have been allocated additional vaccines, others mainly in the eastern and northern regions have performed poorly.
“The Strategic Committee on May 18, in consultation with the Scientific Advisory Committee and the Vaccine Advisory Committee resolved that vaccines be withdrawn from the poorly performing districts to avoid wastage and expiries and that the exercise should commence on May 27.”
Dr. Mwebesa said that three months were given to the districts to utilize vaccines allocated to them so they vaccinate the highly vulnerable groups. This means that the vaccines are due to expire within the next five weeks (around July 10).
“To avoid such a catastrophe, it is extremely important that we withdraw the vaccines,” he said.
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price




