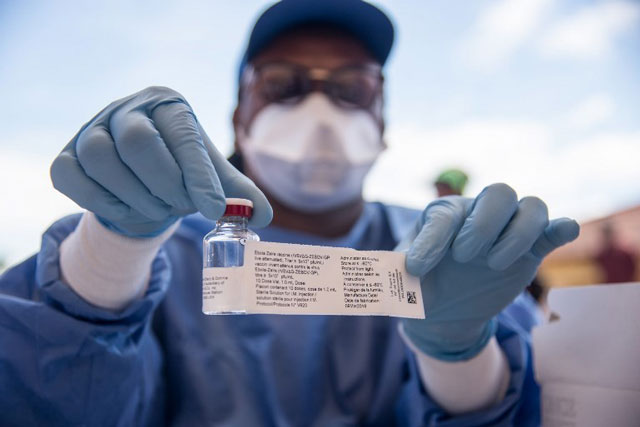
WHO warns big outbreaks becoming `new normal’
The Independent | PATRICIA AKANKWATSA | On June 9, a 5-year old boy travelled from Democratic Republic of Congo (DRC) with his mother after attending a burial of his grandfather who succumbed to Ebola; the deadly hemorrhagic fever.
The grandfather was a pastor who lived in Mabalako Health Zone in Aloya Health Area about 30 km from Beni in DRC. The mother was of Congolese origin but married to a Ugandan and residing in Kasese District in western Uganda. The Congolese mother had travelled back to DRC to nurse her father who had contracted the Ebola virus. Beni and Kasese are about 20km apart.
The health authorities in Beni identified 12 suspect cases from the same family and put them in isolation for monitoring. However, six of the 12 suspect cases escaped and crossed over to Uganda.
Of the six who crossed to Uganda, four were children and two adults with 81 contacts in Kasindi and 40 contacts in Mutwanga, areas bordering Uganda in the DRC. One of the people who crossed over was the wife of the deceased pastor, grandmother to the 5-year old boy.
The child and his family entered the country through the market at Mpondwe bypassing the official border post.
But by the next day, June 10, the boy’s health deteriorated and the mother sought medical care at Kagando Hospital. The child was vomiting blood, had bloody diarrhea, muscle pain, headache, fatigue and abdominal pain.
The clinicians immediately suspected Ebola and transferred him to Bwera where a sample was collected and shipped to Uganda Virus Research Institute (UVRI) for testing. The boy was confirmed positive for Ebola Zaire on the evening of June 11 and he died soon after.
On June 12, his 50-year-old grandmother and three-year-old brother also tested positive for Ebola Zaire. The grandmother succumbed to Ebola too. By the time we went to press, 27 people they came into contact with had been line listed for follow up.
What is being done?
The crossing of Ebola into Uganda has raised a number of issues. Some experts say, with the DRC border where the outbreak has been raging unabated for about a year, it was just a matter of time before cases popped up in Uganda. But others say it should never have happened. On the international scene, there is raging debate about the World Health Organisation (WHO) response to the Ebola outbreak in DRC.
The WHO Director General, Dr. Tedros Adhanom, visited Uganda to assess the Ebola situation and met with President Yoweri Museveni on june 18 at State House Entebbe.
The President assured Dr. Adhanom Museveni said that his government is determined to contain Ebola but the DRC must also deal with the security situation in the Eastern part of that country.
“The issue of security is one of the contributing factors to the spread of the Ebola disease,” Museveni told his guest.
The WHO Director revealed that the efficacy of the Ebola vaccine that was administered to the people that came in contact with Ebola victims, stands at 97.8% success which, he said, is deemed as very good in combating the threat.
He commended Uganda for always being prepared to contain Ebola outbreak whenever it crosses from the DRC.
On June 14, WHO once again controversially refused to declare the outbreak which has killed more than 1400 people, a Public Health Emergency of International Concern (PHEIC).
“It was the view of the committee that the outbreak is a health emergency in the Democratic Republic of Congo and the region, but it does not meet all (the PHEIC) criteria,” Preben Aavitsland, acting chair of an expert committee convened by WHO, said at a press conference in Geneva, Switzerland.
The committee had met for the third time after news emerged that Ebola had spread to Uganda and killed two people. Many infectious disease experts and public officials had expected, and called for, WHO to declare a PHEIC when Ebola broke out of the DRC as that would focus global attention and resources on the crisis.
But who argues that declaring a PHEIC could be interpreted as the outbreak being a global emergency, which could be counterproductive. “As we have seen with previous Public Health Emergencies of International Concern, we risk seeing restrictions on travel and trade, we risk seeing airlines stopping their flights to the area and we also risk border closures,” Aavitsland said.
He said all that could hamper public health efforts in the country which he admitted needs help.
Uganda has been praised for successfully keeping Ebola at bay until now. According to the BBC, the WHO is warning that the world is entering “a new phase” where big outbreaks of deadly diseases like Ebola are a “new normal.”
Dr Michael Ryan, the executive director of the WHO’s health emergencies programme, told the BBC that the world is “seeing a very worrying convergence of risks” that are increasing the dangers of diseases including Ebola, cholera and yellow fever.
He said climate change, emerging diseases, exploitation of the rainforest, large and highly mobile populations, weak governments and conflict were making outbreaks more likely to occur and more likely to swell in size once they did.
The Ebola outbreak in the DRC is the second biggest ever in the world after outbreak in West Africa that hit six countries infected 28,616 people and killed 11,310.
Dr Ryan said as of June 07, the WHO was tracking 160 disease events around the world and nine were grade three emergencies; the WHO’s highest emergency level.
“I don’t think we’ve ever had a situation where we’re responding to so many emergencies at one time. This is a new normal, I don’t expect the frequency of these events to reduce.”
Many hope the case of the DRC family was caught quickly enough to avoid farther spread.
Uganda’s Minister of Health, Ruth Aceng, says Uganda’s response team has been in preparation for the last 10 months and is now in the response phase.
“The Health Ministry is ready to curb the virus,” she says.
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price




