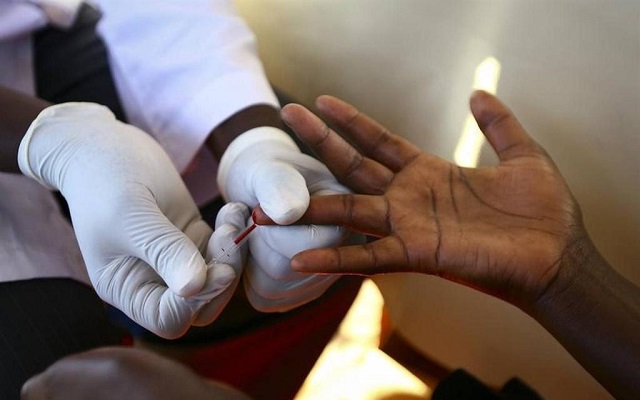
Experts warn of terrible drug resistance as drug stock-outs shake nation
Kampala, Uganda | FLAVIA NASSAKA | July 11, 2012 is memorable for Joseph Lukwago. It is the day the 47-year old started taking Antiretroviral (ARV) drugs. He had tested HIV positive in 2010. And back, he says, thought he had only a short time to live.
After all, he hails from Kalisizo in Rakai district, one of the hardest hit regions of Uganda where the epidemic prevalence stands at 12% – double the 6% national average. Lukwago had known the AIDs story all his life, having lost siblings and a number of relatives to the virus.
In fact, shortly before testing, he had lost a sister and two other relatives to the virus. But thanks to advances in research into treatment, he is still healthy with an undetectable viral load. He says he did not start taking drugs immediately because he was too sick and bedridden.
“Doctors said my CD4 was very low,” he says, “but after some time I was initiated on drugs until now, I’ve never been bedridden again.”
Now, however, Lukwago is not quite sure how long he will be getting the lifesaving drugs. On Oct.31 he was in Kampala in search of drugs after his clinic back in Rakai suffered a stock out. He says he has been getting drugs every three months, but when he went back in September he was given medicine for only two weeks. When he went back, they gave him for four days.
Finally, in October he was told he would be getting a different type because his usual medicine had run out. He says he worried about the new drugs.
“I hear some medicines have serious side effects. My usual dose was only giving me yellow eyes – nothing more,” he says, “I don’t know what this will give me. I am scared of starting it.”
Unfortunately, he could not get his usual medicine in Kampala either. He was told the Ministry of Health had ordered district health officials across the country to reduce HIV drugs refills from the usual three months to two weeks. The ministry did not have money to restock.
In an interview, Dr. Julius Mwijukye, a pharmacist at Masaka General Hospital, told The Independent the National Medical Stores had not supplied certain drugs.
“We have had to make tough choices of substituting patients’ drugs with others,” he says. He is not sure what he will happen to his 400 patients who have been taking the Alluvia drug if the stock out persists.
This comes exactly one year after Uganda endorsed the Test & Treat World Health Organisation guideline in November 2016, requiring whoever tests positive for HIV to be started on ARVs immediately. The country also endorsed that clients will be given 3 to 6 months refills to ensure that patients maintain their treatments.
Now, clinics have since June been reporting either low supplies or complete stock outs of mainly Abacavir/Lamuvidine and Atanazavir for adults in addition to Nevirapine and Lopinavir for children.
The stock-outs have been sometime in coming. Moses Kamabare of the National Medical Stores, a drug procuring entity for government had issued an early warning. In March, he told The Independent that more people had been enrolled on treatment but the budget for these drugs had remained the same.
Endorsing the guideline meant that all the 1.3 million Ugandans living with the virus will be enrolled yet even the 800,000 who were initially on treatment were finding problems getting sustainable supplies due to the same funding challenges.
The government only contributes 7% to AIDs financing and 93% comes from donors; with the US President’s Emergency Plan for AIDs Relief (PEPFAR) being the biggest contributing 62%, Global Fund 28% and other sources 3%.
While he acknowledges the funding challenges, the head of the AIDs Control Programme at the Ministry of Health, Dr. Joshua Musinguzi says “sometimes facilities fail to quantify the exact quantities of medicines they need making patients go without drugs yet they are expiring in the stores”.
But Margret Happy, of the International Community of People living with HIV East Africa (ICWEA), says when patients do not get medicines, it means the country risks failing to meet treatment targets. These include the global 90, 90, 90 targets for countries ensuring that 90% of the people know their HIV status, 90% of those positive to be enrolled on treatment, and 90% these have undetectable levels of HIV virus in their blood.
Dr. John Ssali, the National Medical Director at AIDs Healthcare Foundation – Uganda Cares told The Independent that in addition to patients, erratic stock outs affects programmes of care givers.
“We get first line drugs from government but sometimes they are not there and NMS doesn’t communicate in time. It financially disorganises because we have to arrange buffer stocks,” he says.
He warns that allowing stock outs to continue happening is breeding resistance as drug substitution compromises adherence. For drugs like Nevirapine, Ssali says resistance can be developed with breaks of as few as two weeks.
Currently Ssali’s organization provides drugs to 92,000 patients where 95% are on first line, 4% on second line and 1% on third line drugs. To cater for just those on second line, they spend about Shs483million per quarter and Shs37million for those on third line.
While they use supplies from government to cater for those on first line, the pharmacist says they spend Shs120million on other needs like handling opportunistic infections. If a patient does not respond to certain drugs and test must be done to establish whether its drug resistance, each test for those on first line costs Shs450,000, second line Shs650,000, and third line Shs800,000.
The high cost means that for many patients, the only option when drug stock out happen, is to go home and wait since the government policy is, no health facility should sell ARVs.
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price