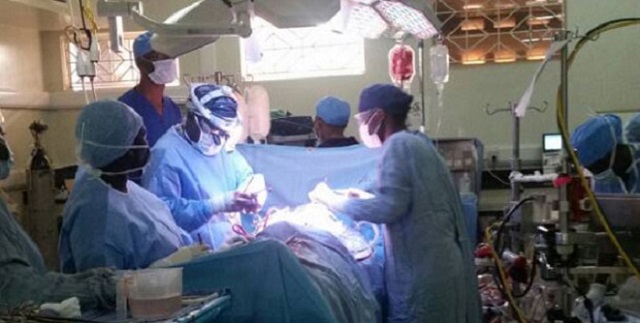
The doctors and the patients tell their story
Kampala, Uganda | FLAVIA NASSAKA | Victor Ndawabo, 58, a Congolese national, was unusually lucky from the moment doctors first discovered he had coronary artery disease (CAD).
The condition which presents with dangerous blockage in the vessels that carry oxygen-rich blood to the heart is often fatal since it tends to develop with few symptoms.
Doctors call it ‘a silent killer’ because some patients – usually older men of 45 years and above— are unaware they have a problem until they suddenly collapse.
They may develop symptoms like palpitations and shortness of breath and crushing pain in the chest (angina) which has been described as similar to someone carrying a heavy weight on the chest.
Doctors say the pain could be made worse by exercise, for instance climbing stairs, but if the blockage is severe, one will get pain even when at rest.
Luckily for Ndawabo, he did not collapse. But he experienced the immense pain in the chest and started finding it almost impossible to get on and off his bed. When he failed to get treatment in his country, he headed to Uganda and the Uganda Heart Institute (UHI).
Doctors at the institute found Ndawabo’s two arteries had been blocked. It was a severe condition and they resolved to conduct a form of surgery called Coronary Artery Bypass Grafting (CABG), which is the third line of treatment in such cases. Normally they would have started with first line treatment—medical therapy—involving taking medicines to control the risk factors for CAD such as high blood pressure and to stop blood clots from forming in the arteries of his heart. If that failed, they would go to second line, which involves procedures that involve putting stents (really gutters) in the blood vessels to keep blood flowing.
But Ndawabo’s condition was so severe that the doctors resolved to conduct the Coronary Artery Bypass Grafting (CABG).
Once again Ndawabo was lucky because this procedure, local medical experts say, would have been impossible in Uganda if he had come to the institute three months ago.
Getting the equipment
Dr William Manyilirah, a consultant cardiothoracic surgeon who led the surgery team says doing CABG requires an Internal Mammary Artery (IMA) Retractor, which allows doctors to lift one half of the patient’s breast bone and gain access to and harvest the affected blood vessel. The Internal Mammary Artery Retractor was only acquired last December and Ndawabo was the second patient to benefit from it.
Ndawabo was admitted for surgery on Jan.31, but a team of 14 experts led by Manyilirah had a week before done the first successful surgery of the kind that involved bypassing three arteries of the heart of a 45-year-old Ugandan patient.
Despite doing several of these procedures in South Africa where he trained for four years, Dr. Manyilirah had not done any in a Ugandan medical facility.
The only time the institute conducted such surgery (a double vessel CABG) was in early 2016. But it was supervised by a visiting South African professor of cardiac surgery and the patient developed complications and had to be taken back to theatre.
The surgery took unusually long because of lack of prerequisite equipment at the time, improvised equipment was used to perform the CABG.
“We didn’t have enough modern equipment. You have to be exceptionally skilled to use the ones they used in 2016,” Manyilirah says.
Another important set of equipment are the micro instruments (dissectors, scissors, and needle-holders, among others), very fine small instruments to handle small vessels.
Manyilirah says the surgery is done in three stages. First, the experts begin by harvesting the grafts (arteries and veins) from the breast bone, forearm or legs. Then they disconnect the heart and lungs and connect them on a heart-lung machine for the surgery. The third stage is the actual grafting (connecting new vessels). Finally, the patient is taken off the heart-lung machine to allow the heart and lungs to function on their own.
“It’s called a bypass because if you got an obstruction here,” he says pointing to a dummy heart he used to illustrate what they did, “We don’t unblock it; we actually put a new vessel.”
In Ndawabo’s case, the surgeons harvested an artery from behind the left half of the breast bone and a superficial vein from the leg and connected it in front of the blockage.
Although it involved arresting the heart and lungs, this was not an open heart surgery but rather doctors worked on the surface of the heart. It appears that after these successes, more patients are lining up for similar procedures.
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price





The Surgery done by the doctors at the Uganda Heart Institute, Mulago exhibited the high level of skill we have as a country. The kind of operation they did has not been done in the East African Region, not event Nigeria and Ghana.
Bravo to the heart surgeons and medical team! Bravo to UHI administration! Bravo to government and the parliamentarians for recognising the great work and supporting the acquisition of more medical equipment and a new home for UHI. This is the way to go.
Appreciating people while they are still alive is a good thing instead of paying tribute to people when they have already died.
Thanks to The Independent team for the quality and informative news. We learn a lot from such stories.