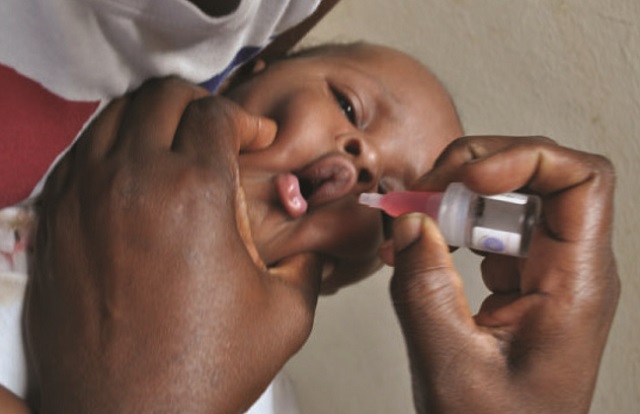
Fate of 1.2 million newborns threatened as prices rise in private clinics
Kampala, Uganda |FLAVIA NASSAKA| It is now official. Uganda is experiencing a shortage of polio and TB vaccines. And Dr. Bernard Opar, the Commissioner Uganda National Expanded Programme on Immunization (UNEPI) at the Ministry of Health who is in charge of immunisation, says “There is nothing much we can do about it”.
“The shortages are a global problem,” he told The Independent.
That is bad news for, especially children who should get the polio vaccine starting at birth. Failure to be vaccinated exposes the child to polio disease, which causes paralysis. Although the TB vaccine is optional, it is highly recommended in Uganda because of the high incidence of TB in the general population.
As anxiety mounts over the fate of children now missing out on these routine immunisations, several options are being offered; including a resort to costly private clinics and use of a more economical administration method called ‘fractional dosing.’
Experts say vaccines are the most effective way to fight off infectious diseases and Uganda has been doing well on it with vaccination rates above 90% for polio and TB. Epidemics have been prevented because they cannot occur if 80 to 90% of the population is immunised.
The Ministry of Health, in a bid to ensure that each child gets the jabs, in 2015 passed a law criminalising anti-immunization sentiments. Also, it was resolved that, in addition to the six killer diseases that children were initially immunised against, they are to get hepatitis B, influenza, pneumonia, and diarrhea shots.
All this success is under threat according Dr. Henry Luzze, a child health expert who commented on the vaccine stock-out. He said best time to vaccinate a child is before they are one year old and delay means that the children are exposed to increased risk of vaccine preventable diseases and yet the country may not be able to handle a potential outbreak of any of the childhood diseases.
The scarcest vaccines are the injectable Inactivated Polio Vaccine (IPV) and BCG for tuberculosis. Dr. Luzze says the oral OPV can be used right from birth, at 6 weeks, 10, and 14 weeks.
The stock-outs are happening barely a year since Uganda launched the IPV in April 2016. According to the Ministry, the IPV contains a killed virus and was designed to avoid the risk of the virus mutating and reproducing that was present when the OPV was used. The OPV contains Polio type 2 virus that carries a risk of mutating into disease.
Dr. Opar is now recommending that anyone who cannot get IPV could just use the oral version OPV. Children can get the oral polio vaccine at birth, at 6 weeks, at 10 weeks and 14 weeks, according to Opar.
But, according to experts, Opar’s desperate recommendation of OPV means that children are not getting immunized against type 2 polio.
Opar also told The Independent that another option would be to ensure that the limited supplies of IPV available are used to serve a bigger number using a technique called ‘fractional dose’. He says this is a highly sophisticated procedure that involves injecting the vaccine in the skin other than injecting it into the muscle. He is wary of introducing the procedure because the country does not have the required trained medical personnel for it.
Mary Nalubega is one of the few nurses who can use the fractional dose technique. She explained that the oral polio vaccine (OPV) creates immunity in the gut unlike the new IPV which creates immunity in the bloodstream. She says IPV offers life-long prevention against polio and urges people to buy the vaccine from private facilities if they can’t find it in government facilities.
But this raises questions of affordability as a package of jabs costs between Shs70, 000 and 140, 000 at the various private health facility accredited by the Ministry to offer immunisation services. The package contains the rotavirus for diarrhea, pneumococcal for pneumonia, and the polio vaccine. Because of the financial costs, some of the estimated 1.2million babies born every year are expected to either go without immunisation or get their jabs late when they are available at a free cost.
The Ministry of Health, in a bid to increase access to services and essential supplies, appointed about 100 health facilities to provide these services free of charge. But even under that arrangement, many were found to be charging patients for the service. According to Opar, many defended the fees as necessary to pay workers and maintain equipment.
Another setback for the vaccination campaign has been that none of the recommendations by Uganda National Immunisation Technical Advisory Group (UNITAG) on new vaccines has been adopted in practice although they got the nod on paper. The group, which conducts research across the country, had found many children to be dying due to diarrhea and meningitis yet a simple shot could have saved them. Formed in 2014 to offer evidence-informed guidance to UNEPI, it has recommended introduction of rotavirus vaccine into the routine immunisation program and meningitis A vaccine for populations in susceptible areas of the country.
But to some experts, the bigger problem is that Uganda relies heavily on donors for most, if not all, solutions to medical problems, including immunisation. Of the Shs38.2 billion that the country spends every year, Shs26billion comes from the Global Alliance for Vaccines and Immunisation (Gavi). According to Luzze, some vaccine stock outs are artificially made by factors that are not streamlined right from the center.
According to Luzze it would be better, even with the limited resources available, if the country improved quantification and distribution from the district stores to health facilities. He said this can put the scarce vaccines to good use to benefit more people.
He says for any private facility to be accredited to provide immunisationservices, it needs to be assessed for human resource capacity in number and knowledge, required cold chain equipment, data collection tools and surveillance capabilities. He says this approach will ensure vaccines are given free of charge as they ought to be.
GAVI has been urging countries to improve their vaccination coverage. According its research, for every dollar invested in vaccines, countries reap up to $16 in economic benefits and up to $44 indirectly.
A recent study also shows that across 94 low- and middle-income countries, the net benefits of averted treatment costs and lost productivity across the life span of immunised groups were worth 16 times the required investment compared to unimmunised people.
Worldwide, according to World Health Organization, 12.9million infants, nearly one in ten infants did not receive vaccination in 2016. Also an estimated 6.6 million infants who did receive their first dose of DTP-containing vaccine did not complete the full, three dose DTP immunization series (DTP3) in 2016. Since 2010, the percentage of children who received their full course of routine immunisations has stalled at 86% (116.5 million infants), with no significant changes in any countries or regions during the past year. This falls short of the global immunisation coverage target of 90%.
****
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price


That is terribly alarming. The government should then get on its marks to manage epidemics of diseases preventable by immunisation.