Stockpiles experimental vaccines for future – Experts
COVER STORY | Independent Team & Agencies | December 05 marked 80 days of responding to the Ebola Virus Disease (EVD) outbreak in Uganda and seven days since the last confirmed case in one of the worst hit districts called Kasanda. A total of 36 contacts were actively being followed-up in four districts, a follow-up rate of 100% in the past 24 hours.
That was a huge relief from mid-to-late October when up to 10 new cases were being reported every day.
Further good news was that eight of the nine districts that had registered Ebola cases had not recorded any new case in the last 21 days. Kagadi district had not registered a new case in over 67 days, Bunyangabo in 66, Kyegegwa in 37, Masaka in 33 and the rest in over 21 days.
The World Health Organisation says for an area to be declared Ebola-free, it should spend 42 days (two 21-day incubation cycles of the virus) without any new cases reported.
That means that Uganda is not yet Ebola free. On Dec.05 14 safe and dignified burials of Ebola fatalities were conducted in Mubende and Kassanda and total alerts validated from districts with active contacts within the past 24-hours were 436, of which 42 met the suspected case definition and 16 were evacuated.
But the Minister of Health, Dr Jane Ruth Aceng has said that if no new case is reported by Dec. 17, then the country will be on the journey to be declared Ebola-free.
On Sept. 20, the Ministry of Health declared an outbreak of Sudan Ebola Virus (SVD) after a case managed at Mubende Regional Referral Hospital (MRRH) in Mubende district was confirmed through testing at the Uganda Virus Research Institute (UVRI). This followed investigations by the National Rapid Response Team of suspicious deaths that had occurred in the district earlier in the month. This is the first time in more than a decade that Uganda reports an outbreak of Sudan ebolavirus.
But on Dec.01, Uganda also announced that all Ebola beds are empty as the last known patient of the Ebola disease had recovered and been discharged from a hospital. Health officials said they hoped that signals that the spread of the virus has slowed dramatically, if not stopped altogether.
“Happy to announce that we discharged the last Ebola patient,” said the Permanent Secretary of the Ministry of Health, Dr Diana Atwine, on Twitter, “God has seen us though this epidemic.”
The last batch of four patients were all at Mubende Hospital. They included three women and a one-year-old baby.
Dr Paskar Apiyo, a consultant physician heading the Mubende Ebola Treatment team said discharging the patients was a milestone.
Mubende Hospital registered 111 Ebola disease patients of whom 62 recovered and 49 died. This was seen as a positive achievement.
“With the experience we have attained here in Mubende, I think if there is another Ebola outbreak in Uganda, more people are going to survive. We are going to write what has been here and it will change the story about Ebola,” said Immaculate Atuhaire.
But, according to some reports, this aggressive containment effort that led to the waning of the outbreak also means a quickly arranged trial of experimental ebolavirus vaccines faces formidable hurdles.
A report by Jon Cohen, Senior Correspondent for the journal `Science’, said the goal of the so-called ring trial is to test the efficacy of the vaccines by giving them to contacts of known cases but the number of potential participants is dwindling fast.
“The plan was to start the trial as soon as early December, but it may have to be called off or redesigned.,” Cohen wrote, “The issue is sensitive, given the amount of effort put into securing vaccines.”
He said roughly $9 million (Approx.Shs33 billion in funding for the trial had been raised and necessary permits obtained.
He said multiple people close to the study—including three Ugandan researchers—refused to speak on the record about the prospects for rolling out the trial vaccines.
But, he added, Mark Feinberg, who heads International AIDS Vaccine Initiative (IAVI), a New York City–based nonprofit that has the rights to a Sudan ebolavirus vaccine, had said, “Whether the study will start or not I think is an open question.”
According to the World Health Organisation (WHO), as of 25 November, Uganda had 141 confirmed cases, 55 of whom had died. WHO tallies include another 22 deaths as likely due to the virus, which had spread, alarmingly, to Kampala, the heavily populated capital.
The last confirmed case was diagnosed on 13 November, save for a stillborn baby on 27 November whose mother had already recovered. After 42 days have passed without a case, the outbreak officially will have ended.
But epidemiologist Mike Ryan, director of WHO’s Health Emergencies Programme, cautioned at a press conference in early December that there were still “significant gaps in tracing some of the chains of transmission,” which means new cases and their contacts may soon surface.
“Ebola always has a sting in its tail,” he said.

Chance to test vaccine
Researchers had hoped for a chance to test new Ebola vaccines. A vaccine has been approved since 2019 for the Zaire ebolavirus, which has caused multiple outbreaks in several countries, including a widespread epidemic in West Africa that ran from 2013 to 2016. But monkey studies suggest that vaccine will not work against the genetically distinct Sudan ebolavirus behind this Uganda outbreak.
In October when Dr Aceng announced that healthcare workers were already testing some new Sudan Ebola treatment options and that three vaccine candidates would be evaluated in the coming weeks, she revealed some details.
She said the initial plan is to gauge efficacy in primary Ebola contacts within 29 days of exposure, with a goal of immunising contacts of 150 confirmed Ebola patients, which would be about 3,000 contacts. She said the trial plans have been finalised and that trials would likely begin in mid-November.
The head of the World Health Organization (WHO), Tedros Adhanom Ghebreyesus, said he welcomed Uganda’s vaccine trial announcement. He added that involving Uganda’s researchers is key to building capacities for safe and effective vaccinations.
When the new Ebola cases surfaced, several vaccines for the Sudan ebolavirus were in development, and Ugandan health officials on 2 December approved testing three candidates. But at the start of the outbreak no manufacturer had enough doses in vials to ship.
The three candidate vaccines recommended for the trial by an independent WHO expert panel include Sabin Vaccine Institute’s ChAd3-SUDV, cAdOx1 biEBOV from Oxford University/Jenner Institute/Serum Institute of India and Merck/IAVI’s SV-SUDV.
To start Phase 3 trials in Guinea during the West Africa Ebola outbreak in 2015, it was 7 months from declaration to arrival of vaccines. This was a great achievement and set historical records at the time. That trial evaluated the safety and efficacy of vaccines against the Zaire ebolavirus—the one responsible for the West Africa outbreak and more recently, outbreaks in the Democratic Republic of the Congo. But there are no licensed vaccines against the Sudan ebolavirus species responsible for the current outbreak in Uganda, thus the need for the current trial.
The trial is led by Uganda’s Makerere University and co-sponsored by the Ministry of Health and WHO. WHO worked with the Ugandan government and researchers to design the protocol for the trial, ensure regulatory and ethical processes were speedy, to train research teams and to install the cold chain that will preserve the vaccines at optimal temperature.
Prof. Bruce Kirenga, the Principal Investigator for the vaccine trial, said nine research teams had been recruited and trained ready to be deployed in the districts where the trial will take place.
“We hope that through the trial we will provide sufficient information to know how effective one or more of the candidate vaccines are, although it will take time to gather quality data,” Dr Yonas Tegegn Woldemariam, the WHO Representative in Uganda. “We are working hand in hand with all partners involved to ensure that the trial will be delivered to high scientific and ethical standards.”
At the time of Cohen’s writing, doses of vaccines developed by the nonprofit Sabin Vaccine Institute and, separately the University of Oxford were expected to arrive in Uganda in a few days.
Cohen said an expert committee organised by WHO says the most promising of the vaccines, originally developed by the Public Health Agency of Canada before being taken up by Merck and then licensed to IAVI, has lagged farther behind because company did not realise until nearly a month into the current outbreak that it had 100,000 old but viable doses frozen in bulk supplies.
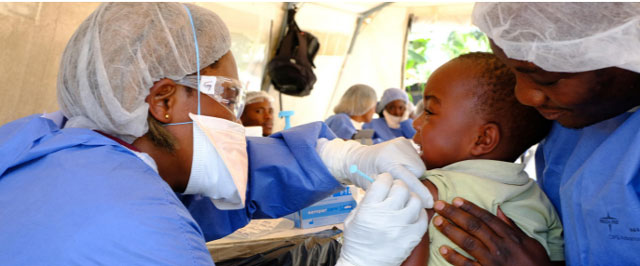
“The vaccines may arrive too late to assess their worth, however,” Cohen wrote, “To be eligible for the ring trial, participants must have been exposed to an infected person within 21 days. As of week two of December, only a few hundred people—about 20 per case—remain eligible. Without new cases, that number decreases each day.”
Ana Maria Henao-Restrepo, WHO’s main representative helping organise the study, said at the early December press conference the trial was “imminent” but had no set launch date.
Even if the ring trial does not launch, Feinberg says he hopes Uganda will stage a phase 1 safety study of the IAVI/Merck vaccine—most likely in health care workers. If it triggers immune responses that mirror the ones seen with the successful Zaire ebolavirus vaccine, the new data, combined with studies that show immunised monkeys have solid protection against the virus, could persuade regulators to approve it for use in future outbreaks.
The Uganda outbreak highlights the need for a more streamlined outbreak response system. “People got these doses together really, really quickly,” says Nicole Lurie, U.S. director for the Coalition for Epidemic Preparedness Innovations—but perhaps not fast enough to save lives. “We need a reserve of (investigational) vaccines so they’ll be at the ready for the next outbreak,” she says.
One answer, says Seth Berkley, CEO of Gavi, the Vaccine Alliance, is to stockpile experimental vaccines on the continent—for Ebola and other emerging diseases—and agree on trial protocols ahead of time. “We have to crack this,” he says, noting that to store COVID-19 vaccines GAVI supplied Uganda and many lower income countries with –80°C freezers that could be repurposed for other vaccine stockpiles.
Berkley acknowledges that creating and maintaining stockpiles would cost money, and it also means periodically throwing away vaccines that expire and replacing them. Still, he says, “It would have been awfully nice to have had 100,000 doses ready to go at the start of this outbreak. That’s where I think we have to go next.”
****
Source: Science
 The Independent Uganda: You get the Truth we Pay the Price
The Independent Uganda: You get the Truth we Pay the Price




